Retention Date: July 30, 2026
Summary of Changes:
This EM replaces the prior version issued on 12/15/2025 and provides updated information and instructions for TAA for Standard Medicare-Only Internet Claims (iClaims).
Section B: Added a note regarding the removal of Remarks from the Medicare-only iClaim.
Section C: Expanded scope of TAA from claims filed within the first 3 months of the Initial Enrollment Period (IEP) to claims filed in the full 7-month IEP.
Section E: Added a note clarifying that claims should not be transferred to MCS from CCE unless a CCE exclusion applies.
Section F: Added a new section about transferring jurisdiction of claims.
Section G: Information moved from section F and added additional guidance on claims with Civil Service involvement. Also added a reminder for technicians to review CCE for pending claims when inquires or documents are received.
A. Purpose
The purpose of this emergency message (EM) is to notify Field Offices (FO) and Workload Support Units (WSU) that Technology Assisted Adjudication (TAA) was released for standard Medicare-only internet claims (iClaims), on December 13, 2025.
B. Background
Previously, Medicare-only iClaims were processed via the Automated Medicare Processing (AMP) application or routed to technicians for review and adjudication through the Modernized Claims System (MCS).
Effective December 13, 2025, TAA will identify “standard” Medicare-only iClaims and process them to completion without any technician intervention in the Consolidated Claims Experience (CCE) system. IClaim applications that do not meet “standard” criteria will be routed to technicians for review and adjudication in MCS or CCE. The criteria for “standard” cases are outlined in section C of this EM.
TAA will automate the processing of standard Medicare-only internet claims (iClaims) by:
· Evaluating the claim to identify discrepancies or edits.
· Checking internal records, including information obtained from Centers for Medicare and Medicaid Services (CMS) data exchanges.
· Identifying policy exclusions and processing limitations, therefore alerting management that technician action is required.
· Generating issues on the Development Worksheet (DWS) in CCE to alert the technician of items that may require additional development (i.e., unauthenticated claims, citizenship, and record discrepancies).
· Routing claims that do not meet the standard criteria to the appropriate office for further development in the CCE or MCS.
· Adjudicating standard Medicare-iClaims to completion. CCE will then establish the MBR.
NOTE: Effective January 31, 2026, the Medicare only iClaim will no longer present the remarks screen to applicants. To review remarks for pending iClaims, refer to Section 3.4 Person Statement in the CCE T2/T18 User Guide.
C. Scope and Limitations
TAA currently has a limited scope and can only complete processing of a claim that meets the standard criteria. For TAA, standard criteria is defined as a claimant who is:
· A U.S. Citizen by birth (not Naturalized citizens) with age and citizenship proven (or tolerance applicable)
· Filing within their 7-month Initial Enrollment Period (IEP)
· Filing for Medicare only
· Filing for themselves on their own record
· Residing in the US with a domestic mailing address
· Selecting English as their preferred written and spoken language
· Fully insured (40 Social Security QCs for Medicare on own record, no Foreign QCs used for insured status)
· Not receiving Medicaid
· Filing for the first time, with no prior:
o MCS segment (active, closed, or deleted),
o iClaim (partial, pending, or completed),
o MBR (under their own or someone else’s SSN), or
o Supplement Security Record (SSR) (under their own SSN)
D. Functionality
Approximately 72% of Medicare only iClaims are now routed to CCE. After TAA successfully processes the Medicare application via CCE, a technician can view:
· The processed claim and development screens in CCE
o The unit code should reflect CCETAA
· The Notice of Award, as well as a copy of the internet application, stored in ORS
· Medicare enrollment information on the MBR or HI/SMI Query Response (HIQR) screen to verify:
o Medicare start dates
o Billing information
o Medicare card issuance
Claims that cannot be processed through TAA will be routed to the WSU/FO of jurisdiction and are accessible in WAC. These claims will be located in two separate folders; Pending Claims and Internet Claims.
IMPORTANT: Offices will need to access the claims in both locations for technician assignment and review.
E. Locating Actionable Claims
Pending Claims
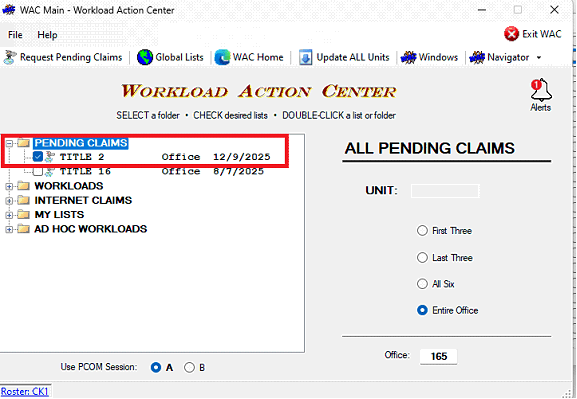 Claims that are unable to be adjudicated by TAA but have successfully been loaded in CCE do not need to be imported. These claims will show on the WAC T2 Pending list with the unit code CCETAA, and a “1” indicator in the MCS column to indicate the claim is located in CCE.
Claims that are unable to be adjudicated by TAA but have successfully been loaded in CCE do not need to be imported. These claims will show on the WAC T2 Pending list with the unit code CCETAA, and a “1” indicator in the MCS column to indicate the claim is located in CCE.
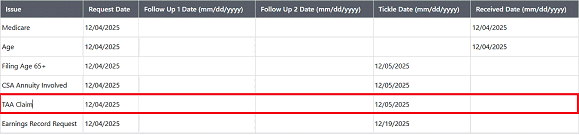
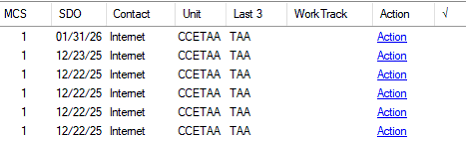 IMPORTANT: Once the claim has been assigned to a technician for review and processing, the unit code should be changed to the typical unit code utilized in the office of jurisdiction. These claims will also have an open Development Worksheet issue of “TAA Claim” which will need to be receipted in upon completion of all outstanding development of the claim.
IMPORTANT: Once the claim has been assigned to a technician for review and processing, the unit code should be changed to the typical unit code utilized in the office of jurisdiction. These claims will also have an open Development Worksheet issue of “TAA Claim” which will need to be receipted in upon completion of all outstanding development of the claim.
 Internet Claims
Internet Claims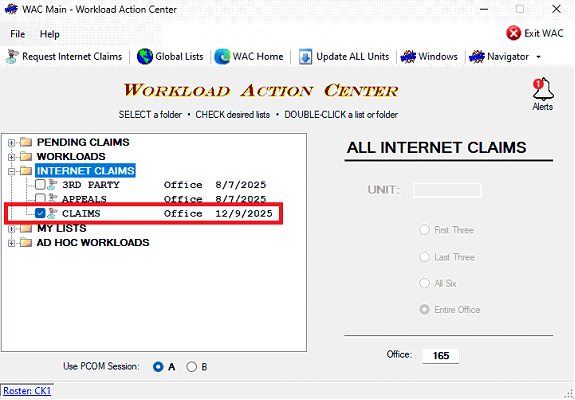 Internet claims that cannot be processed via TAA or CCE will continue to be imported into MCS through normal WAC procedures. Offices should follow normal procedures for importing and assigning cases for review and processing.
NOTE: Claims should not be transferred to MCS from CCE unless a CCE exclusion applies. Any claims transferred from CCE to MCS should not be processed via the Automated Medicare Process (AMP). Processing these claims via AMP could result in processing errors.
F. Transferring Jurisdiction
CCE does not currently have the ability to transfer claims to another office. Technicians should follow existing procedures in GN 01070.781E to determine if the FO or WSU has jurisdiction of the claim. If the claim needs to be transferred to another office, transfer the claim from CCE to MCS, then transfer the MCS claim to the appropriate office.
G. Processing Reminders
Civil Service (CS) Involvement
Technicians should thoroughly review the Informational/Certified Earnings Record System (ICERS) for CS data/CS claim numbers, and/or the earnings record for Medicare for Qualified Government Employment (MQGE) earnings.
Internet claims that cannot be processed via TAA or CCE will continue to be imported into MCS through normal WAC procedures. Offices should follow normal procedures for importing and assigning cases for review and processing.
NOTE: Claims should not be transferred to MCS from CCE unless a CCE exclusion applies. Any claims transferred from CCE to MCS should not be processed via the Automated Medicare Process (AMP). Processing these claims via AMP could result in processing errors.
F. Transferring Jurisdiction
CCE does not currently have the ability to transfer claims to another office. Technicians should follow existing procedures in GN 01070.781E to determine if the FO or WSU has jurisdiction of the claim. If the claim needs to be transferred to another office, transfer the claim from CCE to MCS, then transfer the MCS claim to the appropriate office.
G. Processing Reminders
Civil Service (CS) Involvement
Technicians should thoroughly review the Informational/Certified Earnings Record System (ICERS) for CS data/CS claim numbers, and/or the earnings record for Medicare for Qualified Government Employment (MQGE) earnings.
· If the CS data is not on the ICERS, technicians must contact the claimant to obtain the CS claim number to be added to the claim. If they are in receipt of an Office of Personnel Management (OPM) CS Annuity. SSA is required to withhold Part B premiums from the OPM pension.
IMPORTANT: Civil Service (CS) Claim Numbers Incorrectly Propagating to the HICL Screen
· The DW03 may show a propagated remark for MQGE claims such as, “MQGE 102725102825CSA DATA NEEDED ON HICL?”.
· These numbers will vary. This is not the CS claim number and should not be used on the HICL.
· If there is no CS Annuity, delete any HICL data, and process the claim.
Claim Inquires and Documents
Technicians must review CCE and MCS to determine if there is a pending application when claimants contact SSA, respond to a request for evidence, or submit documents.
Adjudicative Responsibilities
Technicians should follow normal procedures to review and adjudicate the claims that cannot be processed through TAA in CCE and MCS. See GN 00204.059 and GN 01010.008 for technician adjudication responsibilities.
Direct all program-related and technical questions to vHelp, FO management or Program Service Center (PSC) Operations Analysis (OA) staff. PSC OA staff may refer questions, concerns or problems to their Central Office contacts.
Reference:
GN 00204.059 – Internet Claim (iClaim) Medicare-only Application
GN 01070.781 – Field Office (FO) and Workload Support Unit (WSU) Coordination on Claims Processing
GN 01010.008 - Field Office (FO) Adjudicative Responsibilities
HI 01001.020 – Collection of Premiums
MSS25-210 OTH REV 2 - Technology Assisted Adjudication (TAA) - Medicare Internet Claims (iClaims) Release
Consolidated Claims Experience (CCE) User Guide
WAC User Guide